আজ কিছু কমন চর্মরোগের চিকিৎসা সম্পর্কে লিখলাম।
COMMON SKIN DISEASES TREATMENT
Prurigo Simplex :
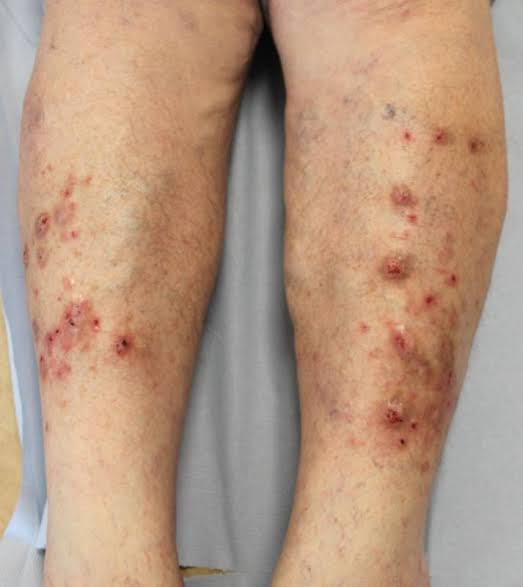
1. Topical Steroid cream
2. Antihistamine, anxiolytic
3. Antibiotic infected
4. Avoid aggravating factors
Impetigo :
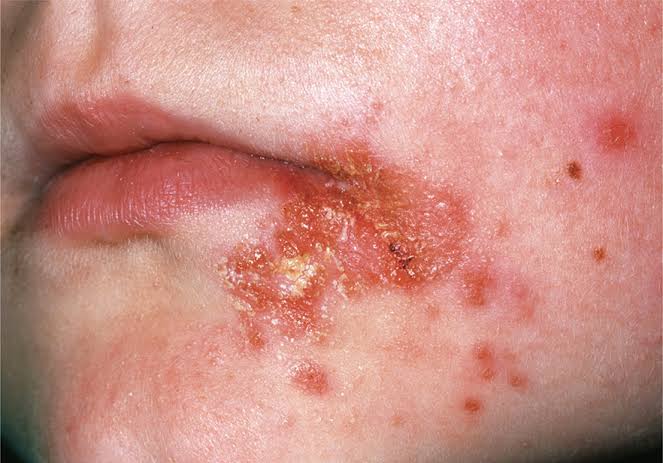
1. Personal hygiene
2. Wound wash by normal saline/ povidone iodine
3. Topical antibiotic
4. Systemic antibiotic
Folliculitis :
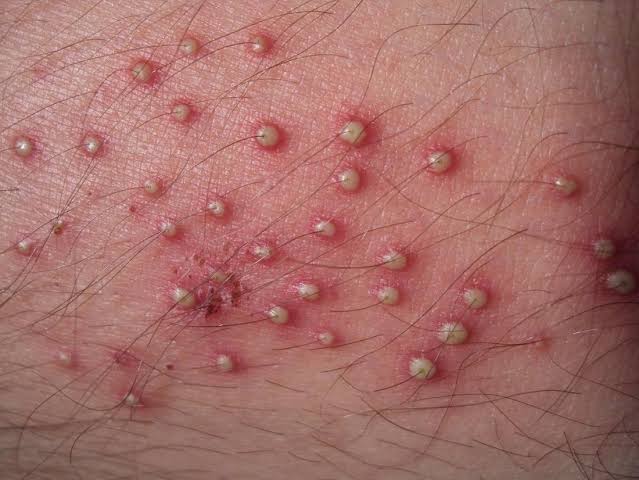
1. Oral Antibiotic
2. Antihistamine
3. Paracetamol
4. Topical antibiotic
Atopic Dermatitis :
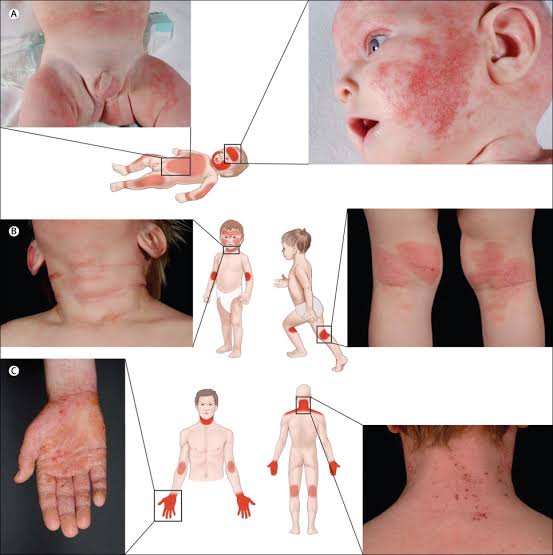
1. Use emollients like vaseline
2. Use moisturising soap
3. Avoid harsh soap
4. Topical hydrocortisone oint. for short duration
5. Oral antihistamine
Scabies :
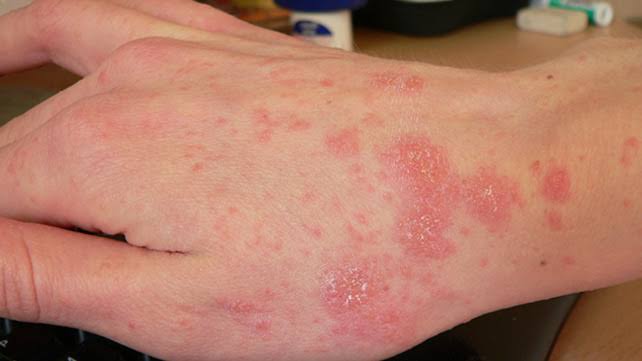
1. Cream for scabies like Permethrin (for 10-12hrs, no need to re-apply) crotamiton/ BB( for 3 consecutive days and need to re-apply 2-3times with a wk apart)
2. All family members should be treated simultaneously
3. Cream should be applied at night, should be kept for at least 10-12hrs.
4. Cream should be after complete control of 2ndary infection usually after 7days.
5. For infected scabies antibiotic
6. All clothings including bed and pillow covers should be boiled and washed by hot water
7. Antihistamine
Oral thrush- Aphthous ulcer :
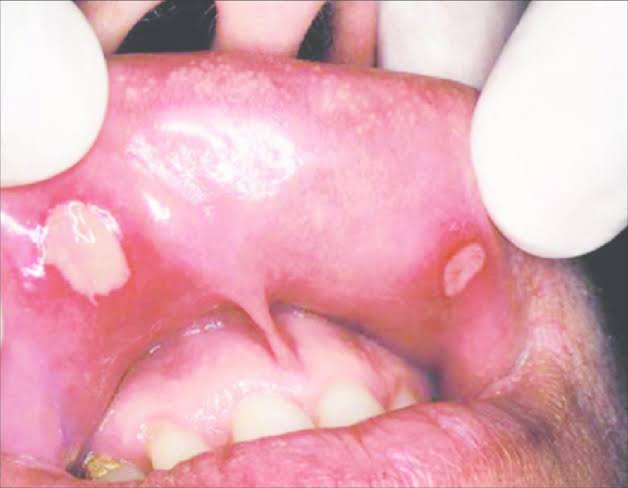
1. Practice good oral hygiene
2. Miconazole gel otherwise Nystatin for Oral thrush can be used
3. Orogel for Aphthous ulcer
4. Rinsing with warm water with salt will also help to relieve pain
5. Avoid spicy food.
Seborrhoeic Dermatitis :
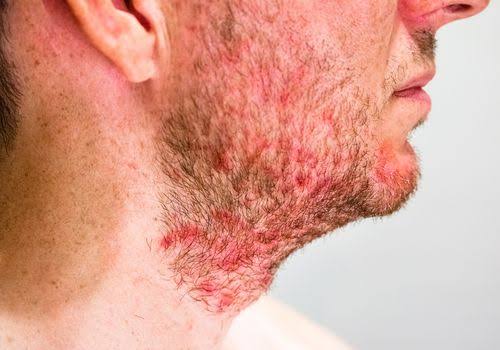
1. Anti-fungal + mild steroid combination cream
2. Anti-fungal shampoo
3. Antihistamine if itching
4. Wash skin regularly
5. Avoid styling skin and hair product
6. To smooth scalp and skin use coconut oil
Pityriasis/ Tinea versicolor :
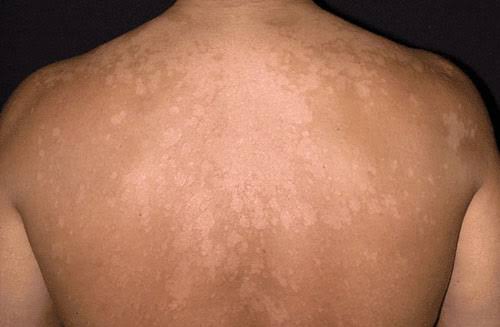
1. Oral antifungal
2. Antifungal cream/ shampoo
3. Ketoconazole soap use during bath
4. If itching antihistamine
5. Avoid sun, use sunscreen
Corn :
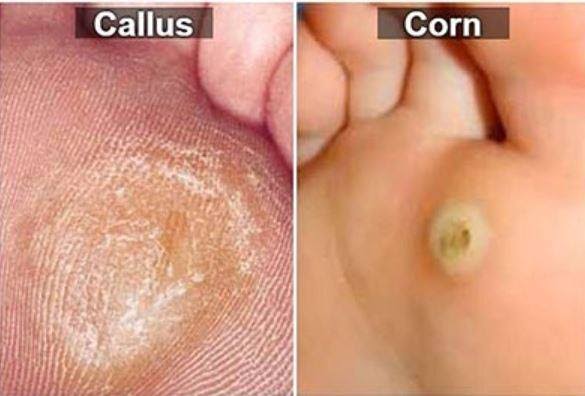
1. Soak ur feet in warm water for soften corn/ callus
2. Moisture the area
3. Apply lotion on corn
4. Apply corn pad to protect the area where a corn or callus developed.
5. Wear comfortable shoes, socks
Cracked sole :
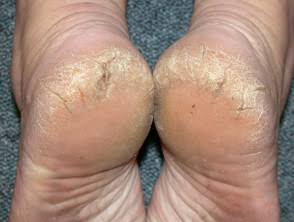
1. Use coconut oil /glycerine/ vaseline on sole
2. Don’t walk without shoe
3. Keep feet in lukewarm soapy water, use footscraber or pumice stone to remove gently hard or thick skin
4. Gently pat your feet dry
5. Apply moisturizer to the affected area
6. Use emollient
7. Wear socks to bed
8. If thickened skin can use keratolytic agent
9. If bleeding or infection use antibiotic
Palmoplantar keratodermas :
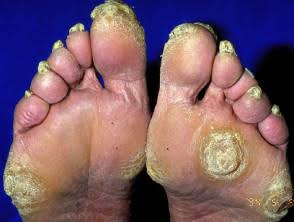
1. Before using topical rx, rinse the foot in lukewarm water to make the sole soft.
2. Use emollient/ oil/ liquid paraffin 2-3times daily.
3. Use keratolytic (salicylic acid) with a moisture (urea) twice daily for 2 weeks.
Using it with occlusion technique helps in better outcome.
4. Avoid walking barefoot
Herpes Labialis & Herpes Zoster :
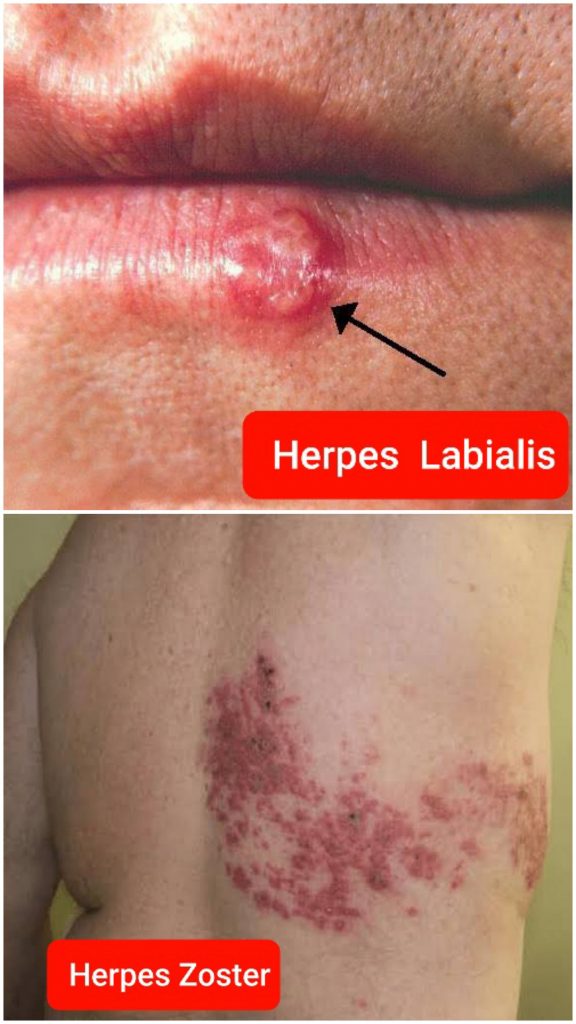
1. Antiviral drug, cream
2. Gabapentin, antidepressant (Herpes zoster)
3. Paracetamol
Dermatitis/ Eczema :
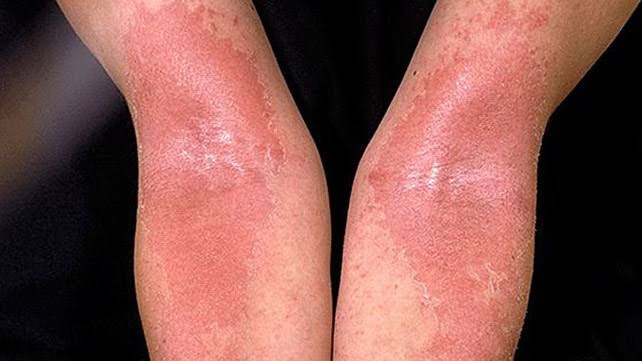
1. Topical steroid
2. Oral Antihistamine
3. Moisture skin
4. Avoid scratching
5. Use anti-itch cream like calamine lotion on affected side
6. Choose mild soap without dyes or perfumes
7. Avoid contacts like food, ornaments, pollen, dust, dyes, perfumes, chemicals which aggravated the condition
8. If infected then antibiotic
Tinea/ Fungal infection :
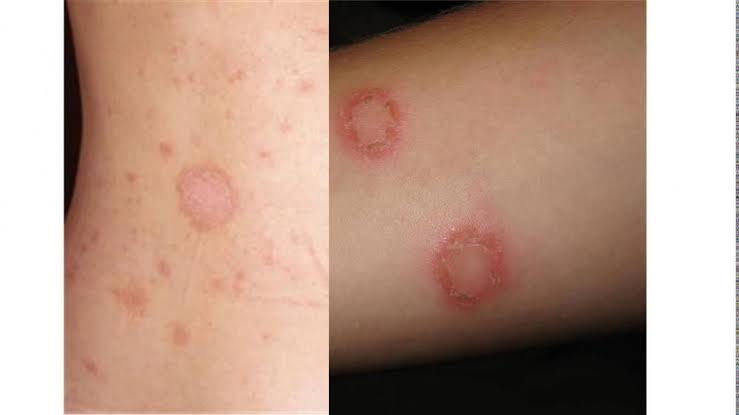
1. Oral Antifungal
2. Topical antifungal
3. Ketoconazole shampoo
4. Antihistamine
5. Wash clothing daily, maintain proper hygiene and avoid tight clothings
6. To find DM
7. Tinea is contagious so don’t share towels, cloths and others
8. After washing, dry the skin throughly like between the toes,groin and the breasts
Acne :
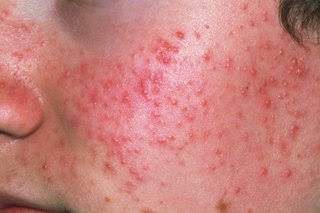
1. Avoid sun exposure, dust, cosmetic
2. Grade1 acne clindamycin lotion good bcz no dryness. RetinA causes dryness so avoid in winter. if It’s indicated u can advice her to use emollients when she feel dry.
3. Antibiotics
4. To avoid triggering factors like OCP, PCOS etc.
5. Avoid oily food, clean face
6. Antihistamine
7. Laser
Melasma :
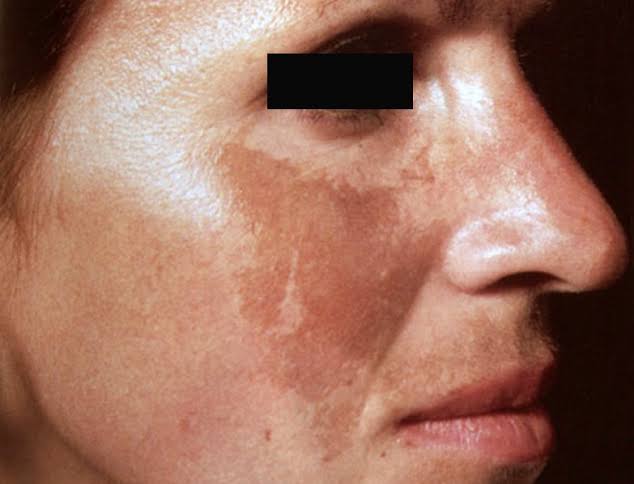
1. Avoid aggravating factor like sun exposure
2. Use sunscreen
3. Topical Fluocinolone + Hydroquinone + Tretinoin
4. History of OCP, thyroid disease should evaluate.
Warts :
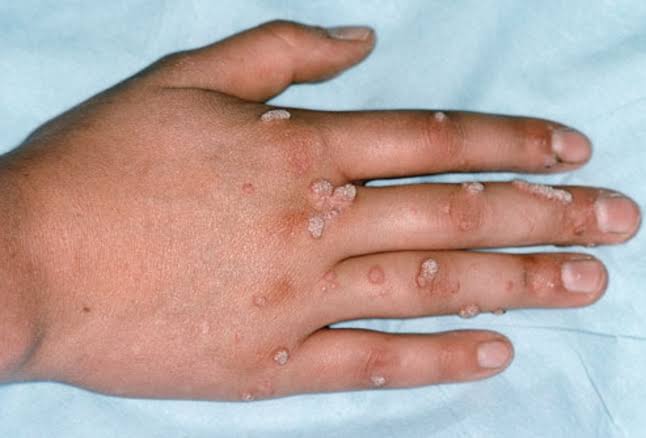
1. Topical
2. Electrocautery/ Cryotherapy/ CO2 laser
FDE (Fixed drug eruption) :
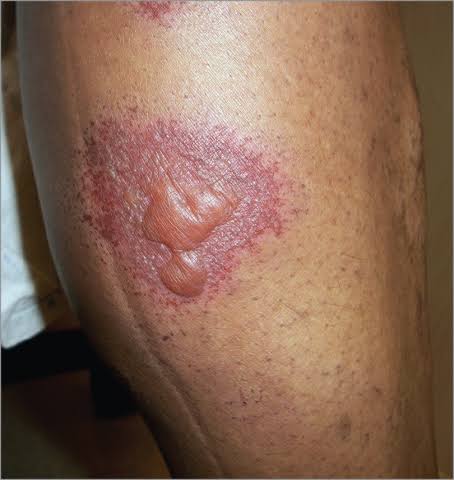
1. Identify the causative agent and avoid it
2. Vaseline
3. If itching antihistamine
4. If infection then antibiotic and wound care properly.
Dr. Tania Hafiz
2003-2004
Z.H Sikder women’s Medical College and Hospital
Working Place::
Caritas Thikana Prokolpo
Arambug, Rupnagar, Mirpur, Dhaka

